Congenital diaphragmatic hernia (CDH) results from developmental defects in the diaphragm, allowing abdominal contents to protrude into the thoracic cavity. Unlike a surgical emergency, it represents a physiological emergency. This condition can lead to persistent pulmonary hypertension and lung hypoplasia, emphasizing the critical nature of its impact on respiratory and overall health.
Immediate treatment for congenital diaphragmatic hernia (CDH) involves stabilizing the newborn’s condition, often including respiratory support and addressing any associated complications. The focus is on managing pulmonary hypertension and ensuring proper lung function to improve the chances of a positive outcome. Bag and mask ventilation can increase air entry into the herniated abdominal cavity, causing further lung compression and compromising respiratory function.
When is surgery typically performed for congenital diaphragmatic hernia?
Surgery for congenital diaphragmatic hernia is typically scheduled once the child’s oxygen saturation stabilizes, and pulmonary hypertension is effectively controlled. This cautious approach aims to create a safer surgical environment by ensuring that the child’s respiratory and circulatory functions are optimized. The stabilization of vital signs is crucial to minimize the risks associated with the surgical procedure and enhance the chances of a successful outcome. This careful timing allows the medical team to intervene when the child is in the best possible condition for surgery, contributing to improved postoperative recovery.
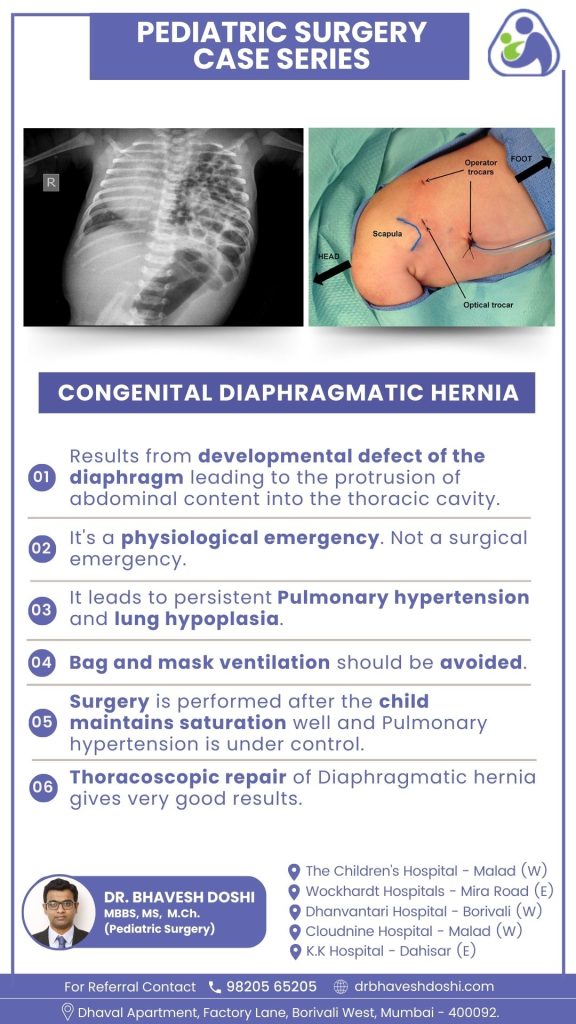
What is the significance of thoracoscopic repair in diaphragmatic hernia cases?
Thoracoscopic repair in diaphragmatic hernia cases holds significant importance due to its minimally invasive nature and associated favorable outcomes. This surgical approach involves making small incisions and using a camera to guide the repair process. The benefits of thoracoscopic repair include reduced trauma to surrounding tissues, minimized postoperative pain, and a shorter recovery period compared to traditional open surgeries.
The minimally invasive nature of thoracoscopic repair contributes to lower postoperative complications, quicker healing, and shorter hospital stays. Additionally, it allows for better visualization of the affected area, enabling precise and effective repair of the diaphragmatic hernia. While the suitability of thoracoscopic repair depends on individual cases, its use is associated with improved overall outcomes and a positive impact on the recovery process for infants with congenital diaphragmatic hernia.
Act swiftly for congenital diaphragmatic hernia (CDH) care. Ensure your newborn’s respiratory health with immediate treatment. Consult now for expert support and a positive outcome.



